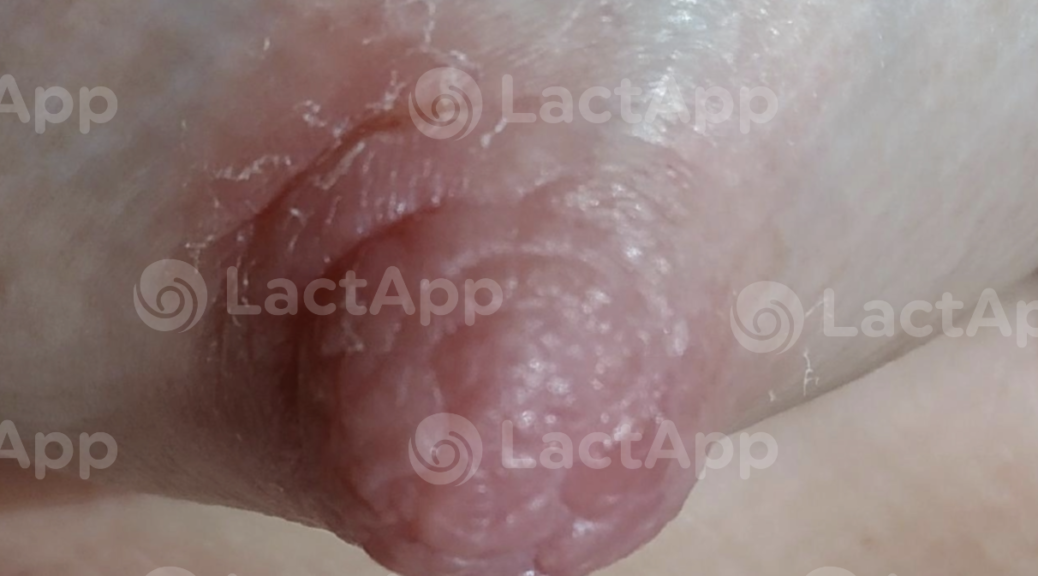
Nipple eczema
Definition
Nipple eczema is an inflammatory skin condition characterized by erythema, inflammation, papules, vesicles, exudates, and crusts. Lichenification, skin erosion, fissures, excoriations, and desquamation can also be observed in the area of the nipple and/or areola.
This definition covers several types of dermatitis (seborrheic and atopic) and irritation or hypersensitivity at contact. In addition, this lesion often occurs concomitantly with Staphylococcus aureus skin infections.
Symptoms of nipple eczema
Symptoms commonly manifested by women who suffer from it are itching, burning, and pain when breastfeeding and when not breastfeeding.
This occurs more frequently when the breastfeeding journey has exceeded seven or eight months of time and it is a pathology that will probably accompany this woman throughout her breastfeeding as it will reappear in the form of outbreaks.
Etiology
Because eczema encompasses different pathologies, there is no common cause for all of them. Therefore, attention must be paid to the possible causes of contact dermatitis, such as soap, creams, patches, breast pads, nursing pads, and so on.
Differential diagnosis
The differential diagnosis must include two pathological processes that may be similar at the beginning:
- Allergic or contact dermatitis. We have already mentioned that eczema could be confused with contact dermatitis. It is advisable to look for the cause of such a reaction.
- Scalded skin syndrome from a staphylococcus aureus infection. In this case, this process may appear before 6 months of the baby’s age. A breast milk culture would be necessary to confirm the diagnosis, and empirical treatment with corticosteroids would be started until the results are available. In the case of eczema, as described below, the response to corticosteroid treatment is rapid. However, scalded skin does not resolve with cortisone but with appropriate antibiotic treatment.
- Paget’s disease. A rare disease associated with breast cancer that starts with a lesion on the nipple, which then spreads to the areola and, at first, can be easily confused with eczema. If eczema treatment gives little response in terms of symptoms, it will be necessary to reconsider the diagnosis.
Treatment of eczema
- Eliminating the allergen if it has become known.
- Initiate topical treatment with corticosteroids. Establish a pattern of progressive withdrawal of topical cortisone treatment to reduce the possibility of recurrence.
- Provide abundant hydration to the affected area. It is important to frequently use moisturizing creams with an emollient effect on the lesion, both simultaneously with the corticosteroid treatment and in the withdrawal pattern up to the following two weeks.
- It’s NOT recommended to frequently wash with soap and water or rub the lesion with gauze or any other product, as it may be counterproductive to the evolution of the lesions.
- Importantly, sometimes, in eczema, there could be overinfection of the lesions and even sores; therefore, it is necessary to assess correctly and add topical antibiotherapy treatment if necessary.
Considerations regarding breastfeeding
- The lesions causing eczema and the treatment for it are fully compatible and safe with breastfeeding, and it is not necessary to stop breastfeeding from the affected breast or discard the human milk.
- If the mother feels pain and prefers to pump temporarily (or stop breastfeeding definitively) from the affected breast, then it is possible to move to exclusive pumping and continue to offer breastmilk expressed from the affected breast or to accompany her in the weaning process.
- The topical treatment should be applied to the affected area after feeding at the breast with a gentle massage. The product should be left for a few minutes to be absorbed before offering the breast to the infant again. If it is impossible to wait, it is advisable to offer the other breast until there are no traces of the product on the nipple or areola.
Nipple eczema is a complication with a good prognosis if adequate treatment is applied and concomitant infections, if any, are controlled. However, it is necessary to inform the mother that this pathology is likely to reappear in time. If she is unaware of this possibility of recurrence, it can generate a situation of frustration. In this way, recurrences, if any, can be detected and treated early.
Bibliography
Barankin B, Gross MS. Nipple and areolar eczema in the breastfeeding woman. J Cutan Med Surg. 2004;8(2):126-130. doi:10.1007/s10227-004-0116-6
Gilmore R, Prasath V, Habibi M. Paget Disease of the Breast in Pregnancy and Lactation. Adv Exp Med Biol. 2020;1252:133-136. doi:10.1007/978-3-030-41596-9_18
Barrett ME, Heller MM, Fullerton Stone H, Murase JE. Dermatoses of the breast in lactation. Dermatol Ther. 2013;26(4):331-336. doi:10.1111/dth.12071