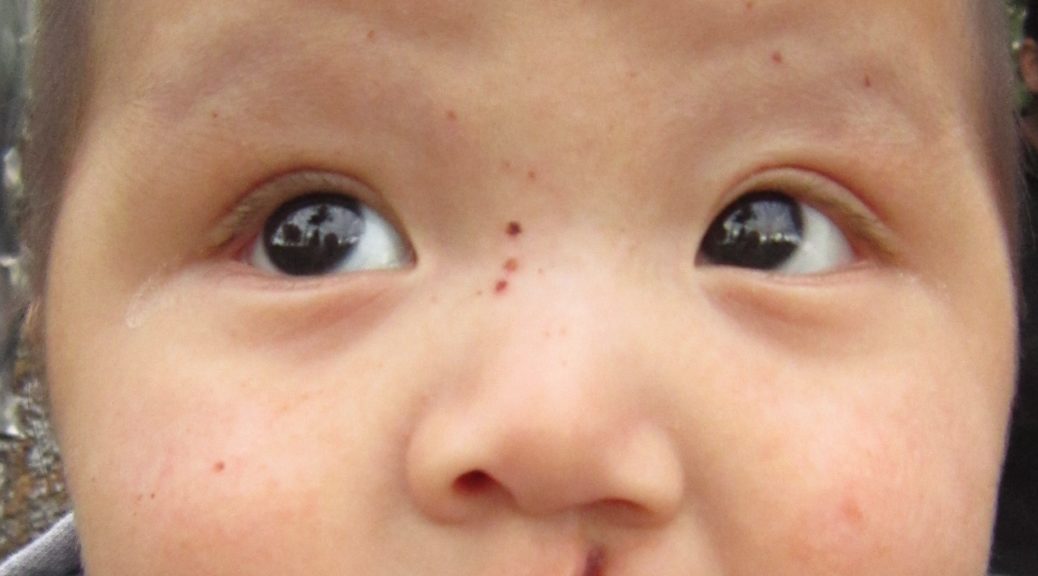
Cleft lip or palate and breastfeeding
How can we maintain (or try to maintain, depending on the severity of the case) lactation in situations of cleft lips, teeth, and palate?
What is cleft lip/palate, and how does it affect breastfeeding?
During pregnancy, the lips are formed between weeks 4 and 7, and the palate between weeks 6 and 9 of pregnancy. Labial, alveolar and/or palatal clefts occur when the tissues that form these oral structures fail to unite.
There is a great variation in the presentation of this type of oral malformation: only the lip can be affected unilaterally or bilaterally, and it can be complete or incomplete depending on whether it affects the nostril (the external opening of the nose), the nasal passage or not.
The same thing occurs in the palate; there are clefts affecting only the soft palate, clefts affecting the soft palate and uvula (the palatine uvula), clefts affecting the hard palate, or clefts affecting the whole structure.
And finally, there are complete clefts that affect the lip, the alveolus (the gums), and the palate, and these can be lateral (affecting the two ends of the lip located below the nose) or unilateral. Sometimes, the presence of a cleft lip and palate can affect the nostrils, partially or semi-partially occluding it, which can make it difficult for the baby to suckle and breathe effectively.
There are many possibilities, so each baby will be different and will require individualized attention regarding breastfeeding. On top of that, there are babies with associated pathologies or syndromes that may also suffer from other oral or facial alterations that hinder breastfeeding, such as retrognathia, micrognathia, macroglossia, and ankyloglossia. An expert assessment is essential before deciding whether to perform surgical correction of the malformation.
In order to suckle, babies need to be able to stabilize the nipple/areola complex in their mouth, seal the breast tissue with their lips and tongue, create a vacuum, and move their tongue toward the roof of their mouth to “milk” the nipple. And when the nipple touches a certain point on the palate, start sucking. If a baby has an orofacial disorder, all these movements can be affected and make it difficult for the baby to latch onto the breast and express milk.
When reviewing the scientific evidence on this subject, this is very unidirectional in that babies with clefts, especially those with cleft palate or cleft lip and palate, cannot suckle. Moreover, some of the studies do not even mention this possibility. Therefore, for a long time, and even now, mothers have been told that breastfeeding will not be possible.
This means that in many cases, no attempt is made to start breastfeeding, or it is “advised” not to try. What we all forget is that children are born to breastfeed, and the birth defect, even though it exists, will not prevent them from trying; and of course, if their mothers have the information and the desire, they are also encouraged to seek information and help to see what options are available.
What difficulties can a cleft lip/palate cause in breastfeeding?
Every case has to be considered on an individual basis, but let’s see in broad outline what difficulties cleft lip/palate can cause:
- Lateral cleft lip: there may be an opening between the breast and the baby’s mouth that prevents the vacuum from being performed inside the mouth.
- Bilateral cleft lip: the main difficulty is that there are two openings that can remain open and make it difficult to perform the intraoral vacuum. In many cases, additionally, this type of cleft may involve a nostril, hindering the breathing process.
- A cleft in the hard palate: The hard palate is the most anterior part of the palate; an opening in this area communicates the nose and mouth, making it difficult for the baby to perform the intraoral vacuum; milk can move to the nose, and breathing can be hindered. The size of the cleft is very variable and will determine, the larger it is, the appearance of other difficulties, such as the baby not being able to “milk” the breast because the tongue does not find the limitation of the palate.
- A cleft in the soft palate: this is the back part of the palate. Sometimes this type of cleft means that the baby also has no uvula, and depending on the affected area, the sucking reflex, which is located between the hard and soft palate, may be absent.
- A cleft in both palates: the defect is so large that it affects the nasal cavity and the nasopharynx. Milk can pass into the nasal cavity, and the baby may have difficulty breathing, maintaining vacuum, and sucking.
- Cleft lip and palate: this is, perhaps, depending on the size of the defect, the most complicated cleft. It affects the lip, the dental alveolus, and the palate. Difficulties may be in the latch, the achieving of the oral seal, the drainage of the mammary gland, and the sucking reflex.
Once the difficulties have been described, let’s see what we can do or propose. Always remember that it will be especially important to be accompanied by a lactation expert with experience in babies with a cleft to facilitate breastfeeding. Because breastfeeding and breast milk (at LactApp, we never talk about the benefits), in these cases, are a treasure:
- The breastmilk that will come into contact with the oral cavity will not cause inflammation because of all the anti-inflammatory components present in breastmilk.
- There is less risk of ear infections (otitis) because if there is a flow of breastmilk through the Eustachian tube, it will not cause inflammation, and the movements that the baby makes when suckling at the breast facilitates the ventilation of the same (regulating the pressure of the middle ear).
- Lower incidence of respiratory pathology.
- The nursing effort will help the baby strengthen the affected oral structures, which will be positive for the subsequent intervention.
- Decrease in the presence of dyslalia when starting to speak.
It should be taken into account that, most probably, when the baby is born with a cleft palate, some type of intervention will be performed on the palate to facilitate the feeding process. Depending on the severity of the situation, there is the possibility that a nasogastric tube will be placed. Usually, a palatal obturator is placed if there is a cleft palate, and in the case of a cleft lip, there are some kind of approximation tapes that allow bringing both ends of the lips closer together.
What can be done to assist breastfeeding in these cases?
There are some basic strategies that can be offered to mothers. At first, they may feel lost and overwhelmed by the situation, but it is important to remind them that they will end up being the best expert on their own baby.
For babies with a cleft lip:
- Find a way to position the baby so that the mother’s breast can close the lip defect. There is no specific position; it will be necessary to look for a position according to the shape of the breast or if the defect is lateral or bilateral.
- The breastfeeding position with the best results is usually the koala hold with a latch in e-dancer to hold the baby’s chin and the breast and cover the defect with the fingers.
- In the case of bilateral clefts, it may be useful to close one of the defects with breast tissue, and for the other one, the mother’s fingers can be used.
- In the case of bilateral wounds, a nipple shield may be helpful. Sometimes, it is necessary to look among the different brands to find one that allows for better coverage of the affected area.
- It is likely that the baby may have some difficulty sucking, so active breast compressions will help the baby get milk more easily.
For babies with cleft palate:
- The first thing that will need to be assessed is whether the baby knows how to or can suck.
- Again, upright breastfeeding positions or rugby hold may work better than others, but we have to repeat that each mother will find the best way to do this.
- In some cases, the biological nurturing position with the mother reclined and the baby fully lying on top will make it easier for the baby to manage.
- Again, nipple shields may be a good idea; in some cases, the nipple shield can compensate for the defect.
- The baby should be kept seated upright as much as possible to prevent milk from passing into the nasal cavity.
- The baby will probably get tired when nursing and may need to receive supplementing with breast milk or formula.
For babies with cleft lip and cleft palate:
- It can be especially challenging to feed a baby with a cleft lip and palate; difficulties present not only with sucking at the breast but also with sucking from a bottle.
- Follow the above guidelines and assess milk transfer.
- If the baby is leaning slightly over the mother’s body, the swallowing reflex will be activated more easily.
- If an effective latch cannot be achieved and, therefore, there is inadequate milk transfer, exclusive pumping (pumping breastmilk and supplementing with another method) can be considered.
- If the baby does not get frustrated, the mother can try to continue to offer the breast in a “pacifier” sucking mode so that the baby benefits from the muscular effort of sucking.
If, despite trying everything, the baby is not able to suck effectively and therefore needs to be fed in another way, it is likely that a bottle with a special teat will be recommended. There are several brands that make teats for babies with cleft lip or palate, with shapes that will help the baby feed according to the defect. If exclusive pumping is chosen, it is recommended that the baby should be offered the bottle very calmly, slowly, sitting up so that their head is higher than their bottom, which will help them to swallow and manage the milk more easily, even if this is more time-consuming and slow. And the baby should not stop sucking the breast, as much as possible: even if it is just for a few times a day and without expressing milk, just to calm down. The sucking they do will be very helpful in the development of the tissues to face the reconstruction intervention that usually takes place between a year and a year and a half of age.
This may seem to be a whole new world, and mothers likely have many doubts about how to do this in each specific case, which is why close follow-up by an expert in this type of situation is essential. Furthermore, for the professionals who assist mothers in these situations, it is essential to know the resources available to offer them.
Do you have further questions?
If you are a lactation professional, our team of experts is available to discuss your cases in the Consultation Channel of the premium version of our LactApp Medical app, available to download for free for Android or iPhone. There, you will also find weekly training with real-world clinical cases to solve each week and much more.